The following is part one of my course notes and findings from Stress, Movement, and Pain.
Linked through the perception of threat and cause to protect, Seth Oberst generously delivered on the hows, whats, and whys between sensation (or lack thereof) and chronic stress. Ultimately, he offered up a framework to identify and mitigate a client’s neurological state. A physical therapist known to dabble in mindfulness, his real mastery is that of human behavior. The two-day seminar filled in every gap and crack left unnamed but felt while working with people.
Those who feel unsafe or disconnected lack the systems and tools for self-regulation.
Self-regulation is the ability to respond to ongoing demands with a healthy range of responses. Neither our internal or external environment is fixed. Nor should it be. To keep us adaptable and tolerant of changing conditions, our energy should flow efficiently from peaks to valleys. This allows us to recover, respond (to future circumstances), and explore a world that is new, alive, and worthy of our efforts.
Artificial self-regulation forms a familiar list: dissociate, distract, and discharge. Stress keeps us stuck in a particular pattern; we don’t have the energy or resources to ‘find another way’. Most fall into the extremes of hypervigilance or collapse. Anxious and overly cautious characterize the first, while frozen conservation depicts the second. We act and behave according to past successes in protecting ourselves.
The Autonomic Nervous System
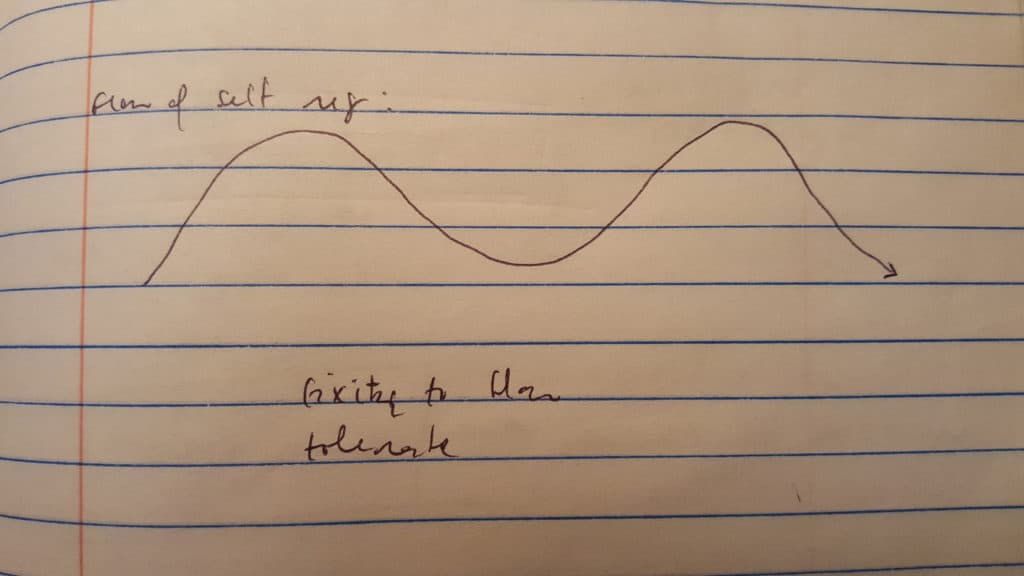
Our subconscious software runs the show. The sympathetic is the ‘fight or flight’, generally referred to as the ‘gas pedal’. The parasympathetic is the ‘rest and digest’, commonly acknowledged as the ‘brake’. In times of threat, the sympathetic keeps us revved and alert. During periods of safety, the parasympathetic eases us back to calm restoration. It ideally flows with rounded curves, mimicking the cycle of self regulation:
The vagus nerve is a really, really big deal when it comes to nuerological regulation. It permeates everything and is both sensory and motor, efferent and afferent. As fish with low oxygen in the water, we were dorsal vagal – freeze and conserve. Once lizards evolved that had to chase prey, the sympathetic (go get it) branch emerged. Social primates developed the ventral vagus branch, connecting the face, heart, and breath. [The polyvagal theory suggests that the idle parasympathetic system actually cleaves into the dorsal and ventral vagal branches.]
Shifting things towards ventral vagal helps override the more primitive systems and promote self-regulation.
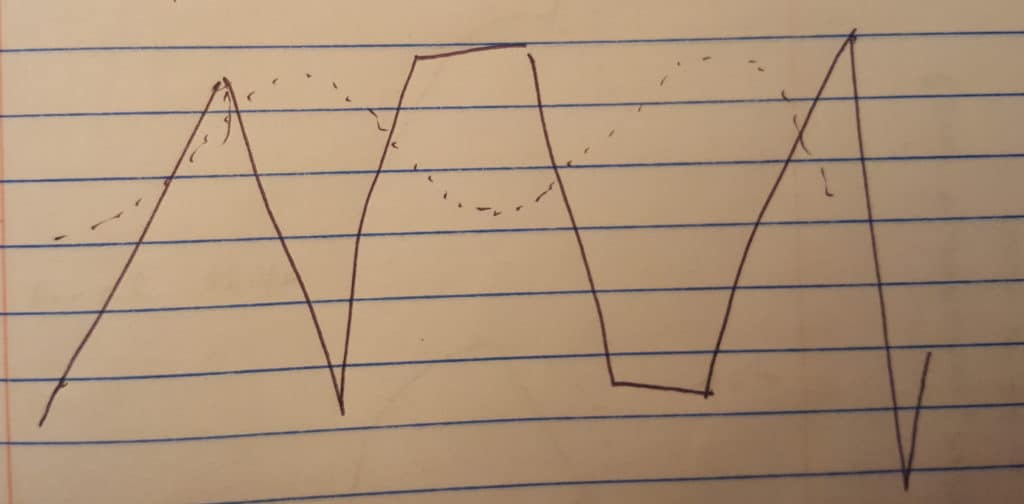 STRESS RESPONSE: Jagged extremes and sticking plateaus versus ventral vagal (dotted line) smoothness.
STRESS RESPONSE: Jagged extremes and sticking plateaus versus ventral vagal (dotted line) smoothness.
The energy-action curve below can help one identify patterns within their internal state. The first change of direction is gradual as action meets energy. The second dips higher instead of drops, marking a sympathetic exchange. The raised peak then plummets below the axis, signifying a dorsal vagal position.
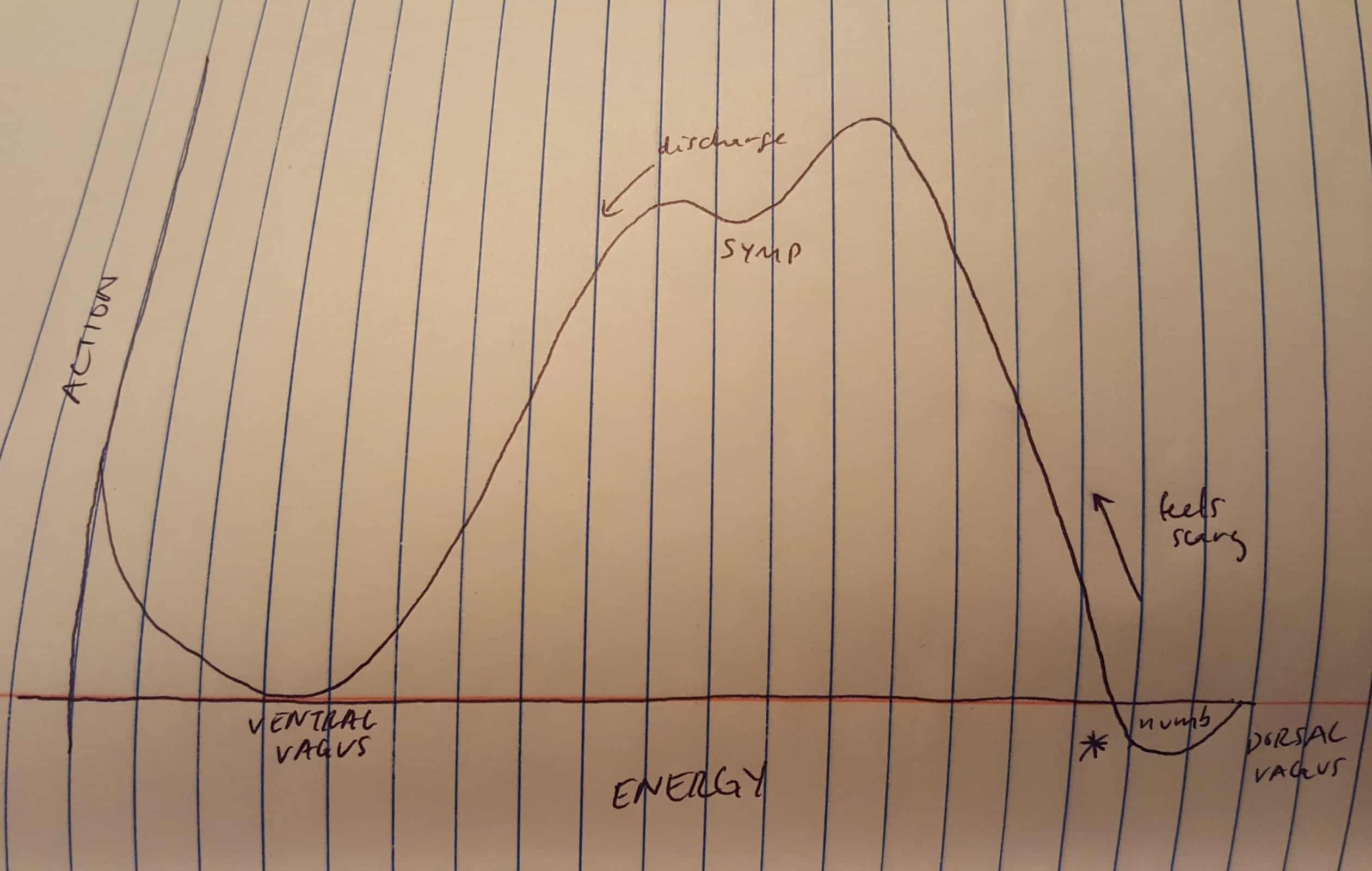
For long term fixes toward an exploratory life, one must REVERSE the curve and work backwards toward ventral vagus. To do so, we have to be willing to acknowledge that things will likely feel worse before they feel better.
Though dorsal vagal may appear to be most passive or apathetic, it utilizes the highest CNS activation. It takes more energy to mask or pretend than it does to exist within the actual feeling. This is why those with dorsal vagal tendencies are exhausted most of the time. They shut down externally to try and keep their internal environment managed and afloat.
Broken down into smaller snippets, sympathetics do more when stressed, commonly to find a semblance of control. In contrast, dorsal vagals do less, typically as little as possible. The up or down shifts are dramatic to try and effect change out of their current ‘crisis’. Anecdotally, Seth reported that about 70% of the clients he sees present sympathetic, while 30% exhibit dorsal vagal signs and symptoms.
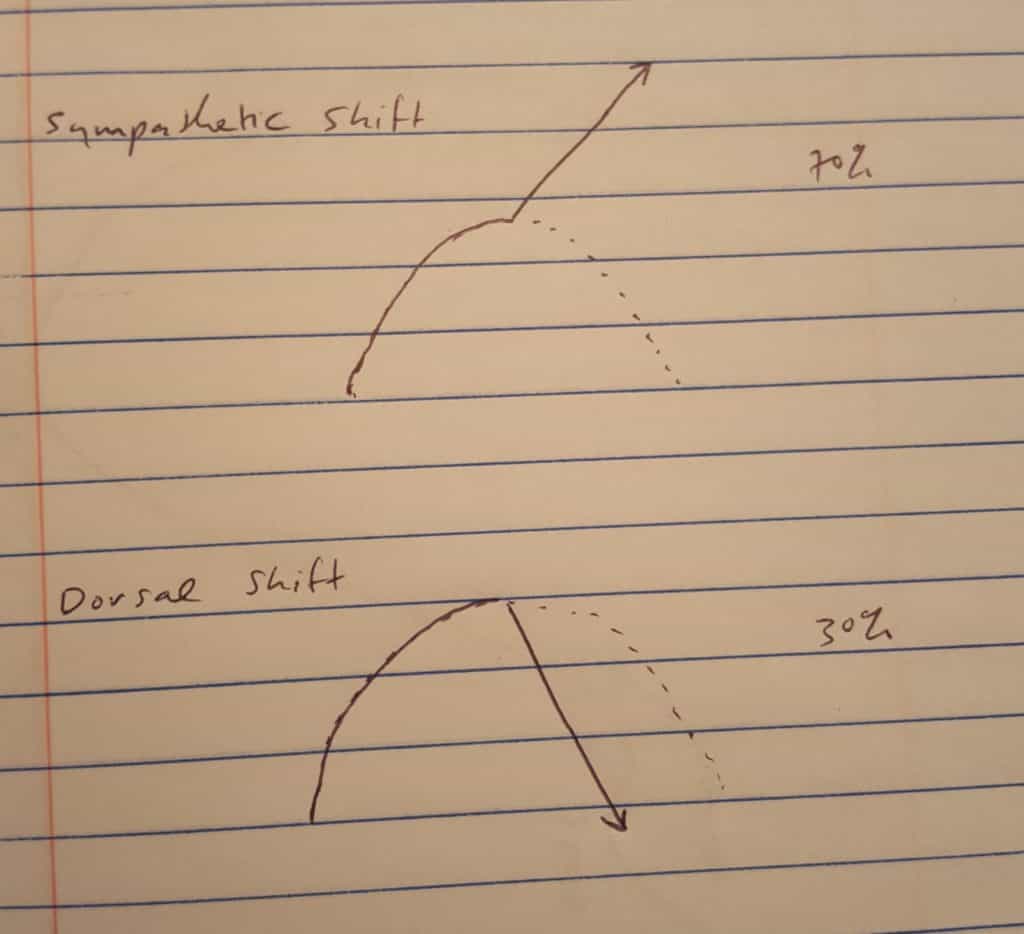
Identifying Neurological Dominance
Story follows state, and words matter. Ventral Vagal will use verbs and adjectives such as fluid, ease, interested, curious, and alive. Dorsal Vagal adopt terms like cold, numb, sluggish, weak, foggy, and tired. Sympathetics talk of being tense, agitated, afraid, anxious, and rigid.
Dorsal vagals walk slumped and unsteady. They are unsure, slower, and tend to drift. These folks need to be coaxed into trying and doing to develop movement confidence. Sympathetics are powerful and almost proud. They take up space and move quickly through it. Adamant and austere, these take charge types want to know what to do and get it done so they can cross it off their list and get on to the next.
The difference between the two is that of intensity. Sympathetics need to relax and settle and become attuned to the subtle signals of the body that come with stillness. Dorsal Vagals need to ‘awaken’, be consistent, and have repeated exposures to progressions. Despite their opposing presentations, both struggle with creating and/or allowing the introspective freedom that promotes investigative movement.
Sympathetics have trouble seeing the point. In their eyes, the conquering is external and the internal is the beautiful power that allows them to do it. They would rather that force remain a mystery. There’s too much to do and take care of to make its unraveling a priority.
Dorsal Vagals feel hopeless about their situation. They’ve resigned to the fact that in doing nothing very little hurts, so they continue to rut into this self-fulfilling prophecy of belief. Convinced that their declining body is a natural occurrence, they determine it is best to go gently into that good night. If movement in general is shied away from, exploration of it is unthinkable.
Part two of this series digs into means and methods of creating a supportive environment and helping clients stay safe and connected within their body.